Adult Periodontitis or Gum Disease
Dentistry primarily treats two major maladies or pathologies of the mouth. Dental caries, or dental decay, is probably the most well known pathology. Another common disease for the dental professional treats is Periodontitis, also known as Gum Disease, Pyorhea or Periodontal Disease, this malody attacks the gums, the bone underlying the gums and the connective tissue which seals the gum tissue to the teeth. Periodontitis is primarily a disease process that results from poor oral hygiene. While some individuals who are diagnosed with this malady may consider themselves to have good oral hygiene, the fact of the matter is that thin layers of tartar or calculus, which begins to form below or at the gumline, creates a rough surface that the patient cannot completely clean no matter how hard they try. Therefore, it is not only those who do not brush or floss who get this malady. Some individuals who are prone to build up tartar (dental calculus) can have below the gum-line tartar "fouling" the roots, making it impossible to clean no matter what the patient does on a daily basis with their oral hygiene.
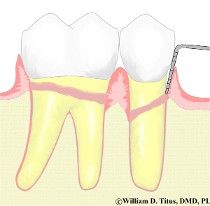
The photo to the right illustrates what happens in the Periodontal D isease process. Calculus retains plaque bacteria under the gumline and creates a chronic inflammation of the gum tissue. This happens because the roughness, created by the tartar, makes it impossible to fully clean the neck of the tooth or its root surfaces the are above the bone level. Floss or toothbrush bristles that sweep under the gum line, and over the rough surfaces, do not fully clean the plaque away. Plaque instead sticks to the tartar. The living bacteria in the plaque, which coats the tartar, stimulates the body's immune system. This stimulation creates a response in the tissues known as inflammation. While inflammation and swelling is not the same, severe cases of inflammation is often seen clinically as swelling (or edema). Swollen gums that bleed easily are said to have gingivitis. If, however, this gingivitis condition persists, and the inflammation begins to break down the bone about the roots, the condition now turns into Periodontitis. The picture to the right illustrates what happens under the gum tissue when periodontitis is present.
To diagnose Periodontitis, one must use an instrument called a Periodontal Probe. This instrument is a straight, thin shaft which has markings in millimeters along it's length. Using this probe, a dentist or hygienist will conduct an exam which measures six points around each tooth in the mouth. The clinician is attempting to determine how far under the gum line the probe can be inserted. Measurements of the sulcus (the collar of tissue about the tooth) should not exceed 3 millimeters in a healthy mouth, and there should be minimal or no bleeding when the probe is removed. When a measurement of 5 millimeters is detected, this can mean, in most cases, that a periodontal pocket is present. Periodontal pockets will almost always bleed when the probe is removed--indicating active inflammation at this site. Bone loss is what allows the probe to reach such a depth, for as the bone is lost, the attachment which defines the bottom of the sulcus, moves down with the bone level.
Once a sulcus reaches 4 to 5 millimeters in depth, the oxygen at the botton of this sulcus is minimal. This provides an excellent environment for anerobic bacteria (bacteria which do not like oxygen). It is this type of bacteria that causes more severe gum inflammation, toxins which invade the tooth structure and also creates malodorous breath.
To diagnose Periodontitis, one must use an instrument called a Periodontal Probe. This instrument is a straight, thin shaft which has markings in millimeters along it's length. Using this probe, a dentist or hygienist will conduct an exam which measures six points around each tooth in the mouth. The clinician is attempting to determine how far under the gum line the probe can be inserted. Measurements of the sulcus (the collar of tissue about the tooth) should not exceed 3 millimeters in a healthy mouth, and there should be minimal or no bleeding when the probe is removed. When a measurement of 5 millimeters is detected, this can mean, in most cases, that a periodontal pocket is present. Periodontal pockets will almost always bleed when the probe is removed--indicating active inflammation at this site. Bone loss is what allows the probe to reach such a depth, for as the bone is lost, the attachment which defines the bottom of the sulcus, moves down with the bone level.
Once a sulcus reaches 4 to 5 millimeters in depth, the oxygen at the botton of this sulcus is minimal. This provides an excellent environment for anerobic bacteria (bacteria which do not like oxygen). It is this type of bacteria that causes more severe gum inflammation, toxins which invade the tooth structure and also creates malodorous breath.
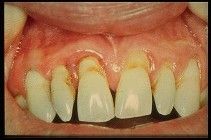
To treat periodontitis one must give the patient a cleansable tooth. Teeth that cannot be fully cleansed of plaque, because of tartar or bone defects, will continue to have inflammation in the gums about them and this inflammation will continue to cause more bone breakdown. Two main methods are used to help the patient obtain a cleansable tooth. The most common method is called scaling and root planning. In this non-surgical procedure, the tartar below the gumline and at the gumline is scraped or vibrated off the teeth. Once the root and crown is glassy smooth, the patient can now floss and remove plaque effectively. If they do this effective plaque removal on a daily basis, the tissues will typically respond well and a significant decrease in inflammation will occur in the gums. When inflammation disappears, swelling decreases and this often results in more shallow probe readings on the gum examination. In some cases, pockets can completely disappear.
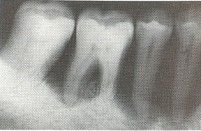
The radiograph to the left illustrates how advanced these bone defects can become. These teeth are hopeless because of the advanced state of bone loss and probably exhibit significant mobility.
The radiograph to the left illustrates how advanced these bone defects can become. These teeth are hopeless because of the advanced state of bone loss and probably exhibit significant mobility.